Hormones and Allergies: Why Symptoms Change During Life
Allergy symptoms do not always stay the same from childhood to adulthood.
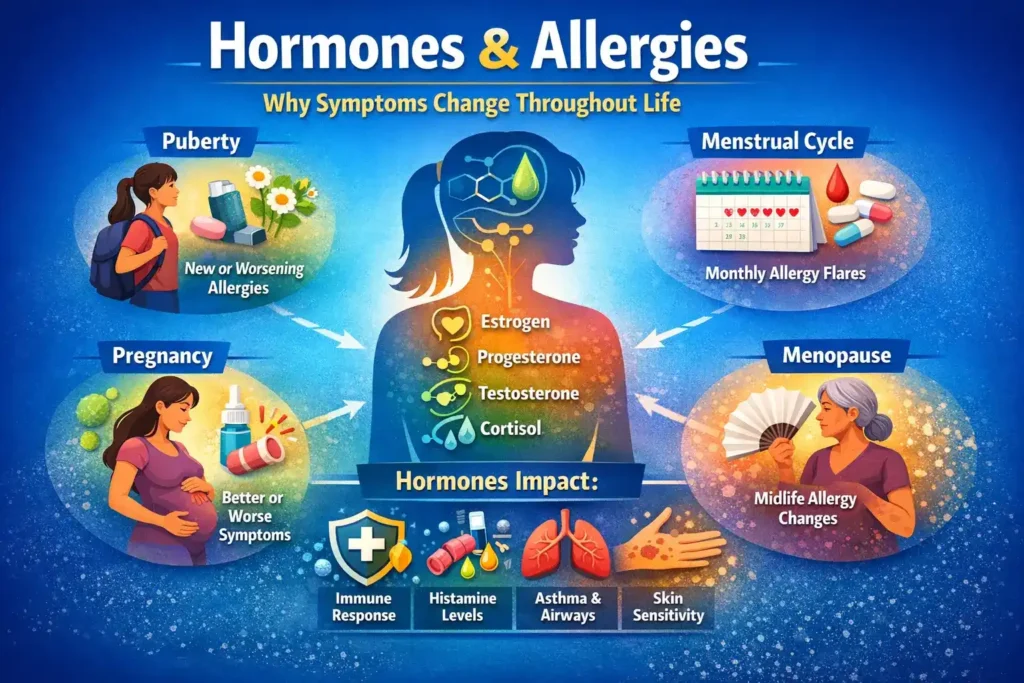
A person who had mild seasonal allergies in school may develop stronger symptoms in their teenage years. Someone with stable asthma may notice flares before menstruation. Another person may feel better during pregnancy, then worse again after delivery. Many women also report new or changing allergy symptoms during peri-menopause and menopause.
These changes are not random.
Hormones can influence how the immune system reacts to allergens, how much histamine is released, how sensitive the airways become, and how strongly inflammation appears in the skin, nose, and lungs (Gutiérrez-Brito, J. A., et al. 2025).
Hormones do not replace the role of pollen, dust mites, mold, food triggers, or environmental exposures. Those triggers still matter. But hormones can change how strongly the body responds to them.
That is why the same allergen may feel more intense at one stage of life and less disruptive at another.
Why Hormones Matter in Allergic Disease
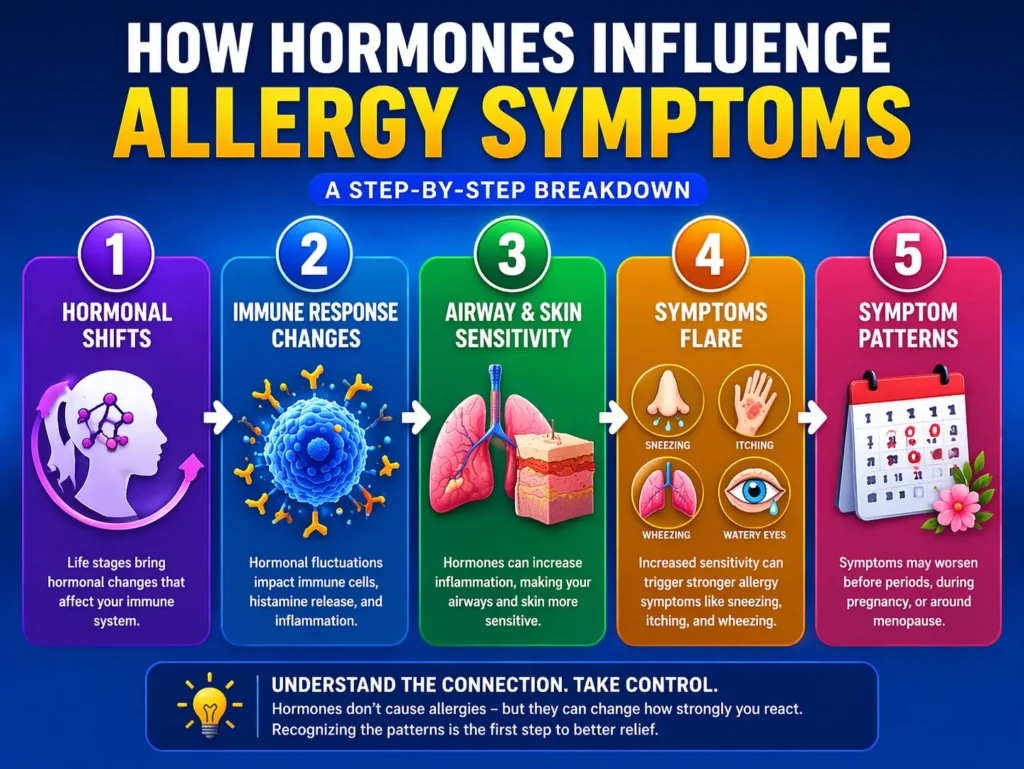
The immune system and the endocrine system are closely connected.
Hormones such as estrogen, progesterone, testosterone, and cortisol do much more than regulate reproduction, menstruation, pregnancy, or stress. They also affect immune cells, inflammatory messengers, blood vessels, mucus production, and tissue sensitivity.
In allergy, that connection becomes especially important because allergic reactions depend on a chain of events involving:
- IgE antibodies
- mast cells
- histamine release
- eosinophils
- airway inflammation
- skin barrier function
- type 2 immune responses
When hormone levels rise, fall, or fluctuate, this allergic pathway can become more active or less stable.
In simple words, hormones can change the body’s “reaction setting.” The trigger may stay the same, but the response to the trigger may become stronger, quicker, or more difficult to control.
How Hormones Affect the Immune System
Estrogen
Estrogen is one of the most important hormones in this topic.
It can enhance several immune processes involved in allergic disease. Research suggests that estrogen may support stronger humoral immune activity, increase mast-cell responsiveness, and contribute to pathways linked with airway inflammation and histamine-related symptoms (Bonds, R. S., & Midoro-Horiuti, T. 2013).
This helps explain why:
- some allergic conditions become more noticeable after puberty
- some women feel worse before their period
- symptoms may shift during pregnancy
- peri-menopause can bring new or stronger reactions
Progesterone
Progesterone has a more complex role.
In some settings, it can calm parts of the immune response. In other settings, rapid hormonal shifts involving progesterone may still contribute to changing symptoms in asthma, rhinitis, or eczema. Its effects can vary by tissue, life stage, and the person’s overall inflammatory profile.
This means progesterone is not simply “good” or “bad” for allergies. Its impact depends on context.
Testosterone
Testosterone and other androgens are often linked with more suppressive effects on some inflammatory pathways. This may partly explain why patterns of allergy prevalence often differ between males and females at different ages.
Cortisol
Cortisol is the body’s main stress hormone.
Under normal conditions, cortisol helps regulate inflammation. But poor sleep, chronic stress, and long-term neuroendocrine strain can make symptoms less predictable and may worsen disease control in people who already have allergic conditions.
The Key Allergy Pathways Hormones Can Change
Hormones influence allergies through several major biological routes.

1. IgE Activity
IgE antibodies are central to many allergic reactions.
When a sensitive person is exposed to an allergen, IgE helps trigger mast cells and other immune cells. Hormonal changes can affect the strength of this response, which may influence how intensely symptoms appear.
2.Mast Cells and Histamine
Mast cells are major players in allergy.
When activated, they release histamine and other chemicals that lead to:
- itching
- hives
- sneezing
- swelling
- wheezing
- watery eyes
- nasal congestion
Hormonal fluctuations can make mast cells more reactive. That is one reason symptoms sometimes flare during hormonal transitions.
3.Airway Hyperresponsiveness
In allergic asthma, airway tissues can become overly reactive.
Hormonal changes may influence bronchial sensitivity, mucus production, and inflammatory balance, which can affect asthma control even when exposure to allergens has not clearly changed.
4.Skin and Barrier Function
Hormonal changes may also influence skin sensitivity and inflammation.
This matters in conditions such as:
- eczema
- contact reactions
- urticaria
- itching without a clear rash
Puberty: The First Major Shift
Puberty is often the first life stage where allergy patterns noticeably change.
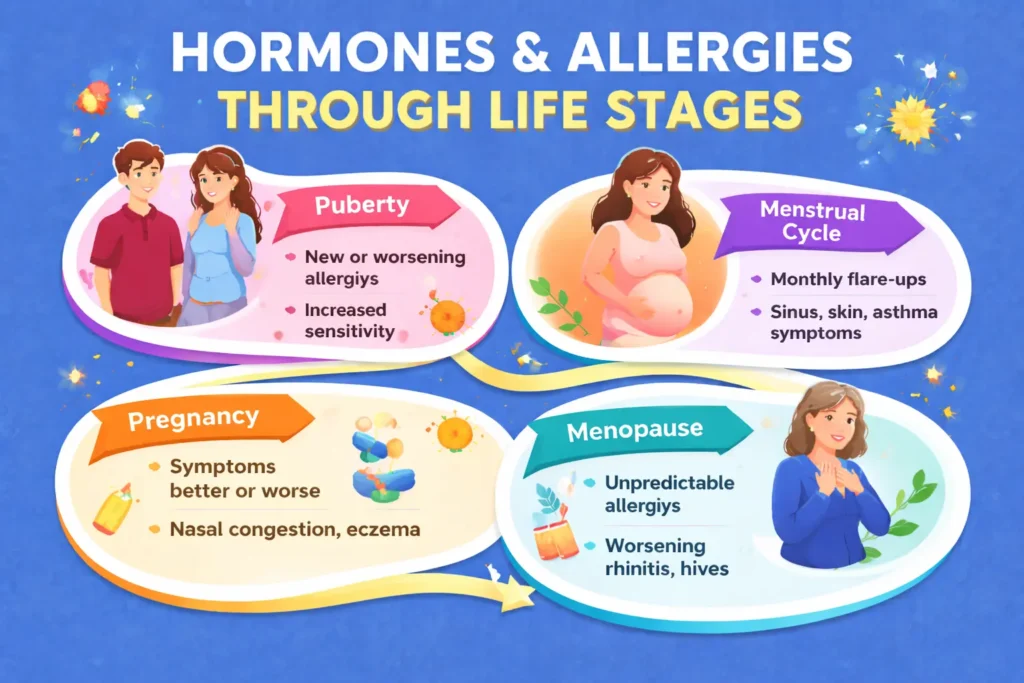
Before puberty, boys may show higher rates of certain allergic conditions. After puberty, girls and women often show greater prevalence or severity in several allergic diseases. This change is believed to be closely linked to hormonal effects on immune regulation (Weare-Regales, N., et al. 2022).
In real life, puberty may bring:
- new seasonal allergies
- worsening nasal congestion
- more visible eczema flares
- stronger asthma symptoms
- increased sensitivity to pollen, pets, or dust
This does not happen to every teenager.
Still, puberty is a major turning point because the hormonal environment changes rapidly, and the immune system responds to that shift.
Menstrual Cycle and Monthly Allergy Flares
For many women, one of the clearest examples of hormones affecting allergies is the menstrual cycle.
Symptoms may worsen during the late luteal or perimenstrual phase, when estrogen and progesterone levels change quickly.
Common cycle-linked complaints include:
- more sneezing
- worse sinus pressure
- increased nasal blockage
- chest tightness
- more coughing
- more itching
- worse hives
- greater rescue inhaler use
This pattern can be easy to miss.
A person may think the problem is weather, stress, poor sleep, or a stronger pollen day. Sometimes that is true. But when symptoms repeat around the same point each month, a hormonal contribution becomes much more likely.
Signs the menstrual cycle may be influencing symptoms
Watch for these clues:
- asthma worsens before menstruation
- hives seem to recur monthly
- rhinitis becomes more severe just before a period
- eczema flares follow a repeating monthly pattern
- regular medicines seem less effective during the same cycle phase
What can help
A symptom diary is often very useful.
Track:
- day of the cycle
- nasal symptoms
- skin symptoms
- breathing symptoms
- antihistamine use
- inhaler use
- sleep disturbance
- exposure changes
Over two to three months, a pattern often becomes clear.
Pregnancy: Better, Worse, or Unpredictable
Pregnancy brings one of the biggest hormonal shifts in adult life.
Estrogen and progesterone rise substantially. The immune system also adapts to support the pregnancy. Because of this, allergy symptoms can move in different directions.
Some people feel better.
Some feel worse.
Some stay about the same.
Pregnancy-related changes may affect:
- allergic asthma
- nasal congestion
- skin sensitivity
- eczema
- swelling
- cough and airway symptoms
This variability is important. Pregnancy does not create one fixed allergy pattern for everyone. Instead, it changes the internal immune environment, and the result depends on the individual.
Why pregnancy changes symptoms
Several factors may play a role:
- immune tolerance shifts
- altered airway sensitivity
- mucosal swelling
- changes in inflammatory signaling
- variable mast-cell behavior
- overlapping reflux or sleep problems
Why close medical review matters
Asthma control during pregnancy is especially important because poor control can affect both maternal and fetal health. If breathing symptoms worsen, it should not be dismissed as “just hormones.” It deserves proper clinical attention (Chong, A. 2025).
The postpartum period also matters
After delivery, hormone levels fall rapidly.
That means symptoms may change again in the weeks or months after birth. A person who improved during pregnancy may worsen postpartum, while another may stabilize after delivery.
Peri-Menopause and Menopause: A Commonly Missed Transition
Peri-menopause and menopause are major hormonal stages, yet allergy changes during this time are still often under-recognized.
Many women report that symptoms become more unpredictable in their 40s or 50s. Some experience stronger allergic rhinitis, new cough, skin irritation, flushing, swelling, or worsening asthma. Others feel that their usual medicines no longer work the same way.
This matters because fluctuating and declining estrogen levels can affect mast-cell activity, inflammatory signaling, vascular responses, and histamine-related symptoms (Valerieva, E., et al. 2026).
What peri-menopause may look like
A person may say:
- “My allergies got worse in midlife.”
- “I never used to react like this.”
- “My skin suddenly feels sensitive.”
- “My nasal symptoms are stronger now.”
- “I’m having new hives or swelling.”
These experiences should not be ignored.
Why menopause can affect allergies
Possible reasons include:
- changing estrogen levels
- altered mast-cell responsiveness
- changes in airway sensitivity
- sleep disruption
- chronic stress
- overlapping age-related conditions
- medication burden
New allergy or changed old allergy
In midlife, symptoms may represent:
- a true new-onset allergic condition
- a worsening of a previously mild condition
- a different expression of existing inflammation
That is why a proper review is important rather than assuming it is only menopause or only allergy.
Why Women Often Notice Stronger Hormone-Linked Changes
Women commonly report more noticeable life-stage shifts in allergic symptoms because hormone fluctuations are broader and more frequent across puberty, menstrual cycles, pregnancy, postpartum changes, and menopause.
Recent work on sex and allergy also highlights that biological sex can influence:
- immune-cell behavior
- inflammatory phenotype
- disease severity
- symptom patterns
- possible treatment response differences (Ventura, M. T., et al. 2025).
This does not mean every symptom difference is caused by sex hormones alone.
Other contributors still matter, including:
- genetics
- environment
- obesity
- stress
- sleep
- microbiome factors
- smoking exposure
- medication adherence
But hormones remain an important part of the explanation.
Symptoms That May Suggest a Hormone-Allergy Connection
A hormonal contribution becomes more likely when symptoms:
- change clearly after puberty
- worsen before menstruation
- shift during pregnancy
- worsen in peri-menopause
- fluctuate without a major exposure change
- show a repeating monthly pattern
- feel more histamine-driven during hormone transitions
Examples include:
- monthly asthma flare-ups
- premenstrual hives
- cyclical rhinitis
- midlife onset of flushing or swelling
- worsening eczema around hormonal changes
- new sensitivity during peri-menopause
What Patients Can Do
If you suspect hormones are affecting allergies, start with observation.
Keep a simple record of:
- symptom days
- menstrual timing
- pregnancy or postpartum stage
- peri-menopausal symptoms
- medication use
- rescue inhaler use
- sleep quality
- stress level
- major allergen exposures
This can help answer:
- Are symptoms truly random?
- Are they tied to pollen, food, dust, or pets?
- Are they linked to hormones?
- Is there overlap with reflux, infection, or anxiety?
This kind of pattern recognition is often the first step toward better management.
What Clinicians Should Keep in Mind
A hormone-linked allergy pattern should be considered when the timeline is strong and repeated.
Important clinical questions include:
- Did symptoms begin or worsen after puberty?
- Do flares cluster around the menstrual cycle?
- Has pregnancy changed asthma or rhinitis control?
- Did symptoms become more severe in peri-menopause?
- Are skin, airway, and swelling symptoms occurring together?
A good evaluation should include:
- detailed time-linked history
- symptom pattern by life stage
- review of current triggers
- medication review
- assessment for comorbidities
- review of pregnancy or menopause status when relevant
What should be avoided
- dismissing symptoms as “just hormones”
- dismissing symptoms as “just anxiety”
- increasing treatment without reviewing timing
- ignoring repeated monthly or life-stage patterns
When Medical Review Should Not Be Delayed
Medical review is especially important if hormone-linked changes involve:
- worsening asthma
- repeated wheezing
- facial swelling
- angioedema
- severe hives
- faintness
- suspected anaphylaxis
- major symptom change during pregnancy
- sudden onset of severe midlife symptoms
These situations need clinical assessment, not guesswork.
Key Takeaways
- Hormones can change how strongly the immune system responds to allergens.
- Estrogen, progesterone, testosterone, and cortisol all interact with allergy-related pathways.
- Puberty, menstrual cycles, pregnancy, postpartum changes, and menopause can all alter symptom patterns.
- The same allergen may cause different reactions at different times of life.
- Tracking symptoms over time can reveal patterns that are easy to miss.
- Hormone-linked changes are real and clinically relevant.
Conclusion
Hormones do not replace allergens as the cause of allergic disease, but they can strongly influence how allergic disease is expressed.
That is why symptoms may intensify after puberty, flare before menstruation, become unpredictable during pregnancy, or change again during peri-menopause and menopause.
The key message is simple:
The immune system does not work in isolation. It is constantly shaped by the hormonal environment.
When hormones shift, allergy symptoms can shift with them.
Recognizing this connection can help patients feel more understood, help clinicians ask better questions, and lead to more accurate, individualized care.
Medical Disclaimer
This content is for educational purposes only and does not replace professional medical advice, diagnosis, or treatment. If you have severe, worsening, or unusual allergy symptoms, or think your symptoms may be linked to hormonal changes, consult a qualified healthcare professional for individualized care.
Frequently Asked Questions (FAQs)
1. Can hormones really make allergies worse?
Yes. Hormones can affect the immune system, histamine release, and inflammation, which may make allergy symptoms stronger at certain stages of life.
2. Why do allergies change during the menstrual cycle?
Hormone levels rise and fall throughout the cycle. These shifts can trigger changes in nasal symptoms, skin reactions, and even asthma control in some women.
3. Can pregnancy change allergy symptoms?
Yes. Pregnancy can make allergies better, worse, or more unpredictable because it causes major hormonal and immune changes.
4. Why do some women get worse allergies during menopause?
During peri-menopause and menopause, estrogen levels fluctuate and decline. This can affect histamine response, inflammation, and symptom intensity.
5. How can I tell if my allergies are linked to hormones?
Look for a pattern. If symptoms worsen before periods, during pregnancy, or around menopause, hormones may be playing a role. A symptom diary can help identify this connection.
References
- Gutiérrez-Brito, J. A., Lomelí-Nieto, J. Á., Muñoz-Valle, J. F., Oregon-Romero, E., Corona-Angeles, J. A., & Hernández-Bello, J. (2025). Sex hormones and allergies: Exploring the gender differences in immune responses. Frontiers in Allergy, 5, 1483919. DOI: 10.3389/falgy.2024.1483919
- Weare-Regales, N., Chiarella, S. E., Cardet, J. C., Prakash, Y. S., & Lockey, R. F. (2022). Hormonal effects on asthma, rhinitis, and eczema. The Journal of Allergy and Clinical Immunology: In Practice, 10(8), 2066–2073. DOI: 10.1016/j.jaip.2022.04.002
- Ventura, M. T., Costantino, M. T., Crivellaro, M. A., Giuliani, I. M. R., Losa, F., et al. (2025). Gender and allergy: Mechanisms, clinical phenotypes, and therapeutic response—A position paper from the Società Italiana di Allergologia, Asma ed Immunologia Clinica (SIAAIC). International Journal of Molecular Sciences, 26(19), 9605. DOI: 10.3390/ijms26199605
- Valerieva, E., Vasileva, M., Baynova, K., Krusheva, B., Petkova, E., Nenova, M., Novakova, P., Staevska, M. T., Cimbollek, S., & Valerieva, A. (2026). Women hormones and hypersensitivity: Allergic diseases in menopause. Frontiers in Allergy. DOI: 10.3389/falgy.2026.1777688
- Chong, A. (2025). Sex hormones in allergic disease: Overview and spotlight on asthma in pregnancy. Journal of Women’s Health, 34(7), 963–965. DOI: 10.1089/jwh.2025.0170
- Bonds, R. S., & Midoro-Horiuti, T. (2013). Estrogen effects in allergy and asthma. Current Opinion in Allergy and Clinical Immunology, 13(1), 92–99. DOI: 10.1097/ACI.0b013e32835a6dd6

