Allergies vs COVID: How to Tell the Difference
Written by: Dr.Muhammad Ihsan Ullah, PhD
Medically reviewed by: Dr. Jamal ud Din Khan, FCPS
Last updated on April 01,2026

A runny nose, sneezing, sore throat, congestion, or cough can make anyone stop and wonder:
Is this allergies or COVID?
It is a fair question. The two can look similar at first, especially when symptoms are mild. Both can affect the nose, throat, and upper airways. Both can also cause congestion, cough, headache, fatigue, and throat irritation. That is why so many people feel unsure in the first day or two of symptoms.
Still, allergies and COVID are not the same.
Allergies happen when your immune system reacts to triggers such as pollen, dust mites, mold, or pet dander. COVID-19 is a viral infection caused by SARS-CoV-2. One is an allergic response. The other is an infection. That difference shapes the symptom pattern, the level of risk, and the next steps you should take.
The easiest way to tell them apart is not by looking at one symptom alone. It is by looking at the whole pattern.
In general, itching, watery eyes, sneezing, and trigger-related flare-ups point more toward allergies. Fever, sudden loss of smell or taste, body aches, and a more “whole-body” sick feeling point more toward COVID (Sarhan, R. M., et al. 2021).
Why allergies and COVID can feel similar

The confusion usually starts because the two conditions share several symptoms.
Both can cause:
- runny nose
- nasal congestion
- sore throat
- cough
- headache
fatigue
That overlap is real. Mild COVID can sometimes look like a simple upper-respiratory irritation in the beginning. Allergies can also leave people feeling tired, uncomfortable, and congested enough to worry that something more serious is going on.
But once you look beyond the overlap, the differences become much clearer.
Signs that point more toward allergies

If your symptoms are led by itching, allergies move much higher on the list.
Common allergy clues include:
- itchy eyes
- itchy nose
- itchy throat
- watery eyes
- frequent sneezing
- clear nasal discharge
- symptoms that start after pollen, dust, mold, or pet exposure
- symptoms that return during the same season each year
This pattern fits seasonal allergies much more closely than COVID. Allergies are also more likely when symptoms begin after being outdoors on a high-pollen day, cleaning a dusty room, or spending time around a known trigger (Yang, X., et al. 2023).
Itching is especially important. That is one of the biggest real-life clues. Allergies often make the eyes, nose, and throat feel irritated or itchy because the body releases histamine as part of the allergic response. COVID does not usually create that same kind of itch-dominant pattern.
If the main story is “my eyes are itchy, I keep sneezing, my nose is running, and this happens every spring,” allergies are much more likely.
Signs that point more toward COVID
COVID is more likely when symptoms feel more like an infection than an irritation.
Common COVID clues include:
- fever
- chills
- body aches
- dry persistent cough
- sudden loss of smell
- sudden loss of taste
- shortness of breath
- nausea or diarrhea
- strong fatigue or weakness
Clinical comparisons have found that fever, dry cough, shortness of breath, diarrhea, and loss of smell or taste are much more common in COVID than in allergic rhinitis (Sarhan, R. M., et al. 2021).
Fever is one of the most useful signs here. Allergies can make you miserable, but they do not usually cause fever. If a fever appears, that should shift your thinking away from simple allergies and more toward an infection.
The same goes for sudden smell or taste loss. Allergies can reduce smell if the nose becomes blocked, but COVID-related smell loss is often more sudden and more noticeable. It can happen even when congestion is not severe, which makes it an especially important clue (Mitchell, M. B., et al. 2023).
The three most helpful clues
If you want a simple way to sort this out quickly, focus on these three things:
1.Fever
Fever strongly favors COVID over allergies. Allergies may cause tiredness and poor sleep, but fever points much more toward infection (Sarhan, R. M., et al. 2021).
2.Itching
Itchy eyes, itchy nose, and itchy throat strongly favor allergies. That kind of symptom pattern is much more typical of allergic inflammation than viral illness (Yang, X., et al. 2023).
3.Sudden loss of smell or taste
A sudden change in smell or taste deserves extra attention because it is much more strongly linked with COVID than with simple seasonal allergies (Mitchell, M. B., et al. 2023).
Symptom-by-symptom comparison
Runny nose and congestion
Both allergies and COVID can cause a runny nose and nasal congestion.
With allergies, the mucus is often clear and watery. Sneezing and itching are usually present too. With COVID, congestion may come with fever, fatigue, body aches, or smell loss. The congestion itself is not enough to tell the difference, so the surrounding symptoms matter more.
Sore throat
A sore throat can happen with both conditions.
With allergies, it often comes from postnasal drip and repeated throat clearing. With COVID, it may feel more like part of a broader illness. If the sore throat appears with fever, body aches, or a dry cough, COVID becomes more likely.
Cough
Allergies can cause coughing because postnasal drip irritates the throat.
COVID is more likely to cause a dry, persistent cough, especially when it comes with other infection-related symptoms. A cough by itself is not enough to make the call, but a dry cough with fever or fatigue should not be brushed off (Sarhan, R. M., et al. 2021).
Headache
Both can cause headache.
Allergies tend to cause pressure-type headaches, especially when the sinuses feel blocked. COVID may cause headache as part of a more general viral illness. So again, the surrounding symptoms matter more than the headache alone.
Fatigue
Fatigue can appear in both conditions, but it often feels different.
Allergy fatigue is usually linked to congestion, poor sleep, and long-lasting irritation. COVID fatigue is more likely to feel heavier, more sudden, and more “whole-body.”
Shortness of breath
Shortness of breath should always be taken seriously.
Allergies may cause breathing discomfort, especially in someone who also has asthma. But shortness of breath is also a known COVID symptom and deserves prompt attention, especially if it is getting worse (CDC, 2025).
Timing matters more than many people realize
The timing of symptoms can tell you a lot.
Allergies often follow a pattern:
- they appear during certain seasons
- they flare after exposure to pollen, dust, mold, or pets
- they improve when the trigger is removed
- they often come back in the same way each year
COVID does not usually follow that pattern.
COVID is more likely when:
- symptoms appear suddenly
- the symptoms feel different from your usual allergies
- you were recently around someone who was sick
- fever, body aches, or smell loss develop early
That is why the question is not just “what symptoms do I have?” It is also “when did they start, what triggered them, and does this feel like my usual pattern?” (Yang, X., et al. 2023).
How long do allergies last compared with COVID?
Allergies can last for days, weeks, or even months if the trigger remains around you. Someone with pollen allergies may feel bad throughout a season. Someone exposed to dust or pet dander may keep having symptoms as long as the exposure continues.
COVID usually behaves more like an acute illness. Symptoms often develop over a shorter period and then improve over days to a couple of weeks, though some problems, especially smell changes, can last longer in some people (Mitchell, M. B., et al. 2023).
A simple way to think about it is this:
- ongoing, trigger-linked symptoms without fever suggest allergies
- a new illness with fever or sudden smell loss suggests COVID
Can you have both at the same time?
Yes, and that is one reason people get confused.
A person with seasonal allergies can still get COVID. Having allergies does not protect you from infection. In fact, if you already expect certain symptoms every season, it can be easy to miss the moment when something has changed.
That is why it is important to pause and reassess if your symptoms feel different than usual. If you normally get itchy eyes and sneezing but now you also have fever, body aches, or sudden smell loss, it is worth taking that change seriously (Chen, C., et al. 2024).
When should you test for COVID?
You should think more seriously about testing when the symptoms do not match your usual allergy pattern.
Testing becomes more important when:
- fever is present
- smell or taste changes appear suddenly
- symptoms feel different from your usual seasonal allergies
- you had a recent exposure
- body aches or chills develop
- shortness of breath appears
- you feel clearly sick rather than simply irritated or congested
Symptoms alone can help point you in the right direction, but they do not always give a final answer. If there is real uncertainty, testing is often the safest next step (CDC, 2025).
A quick way to think about it
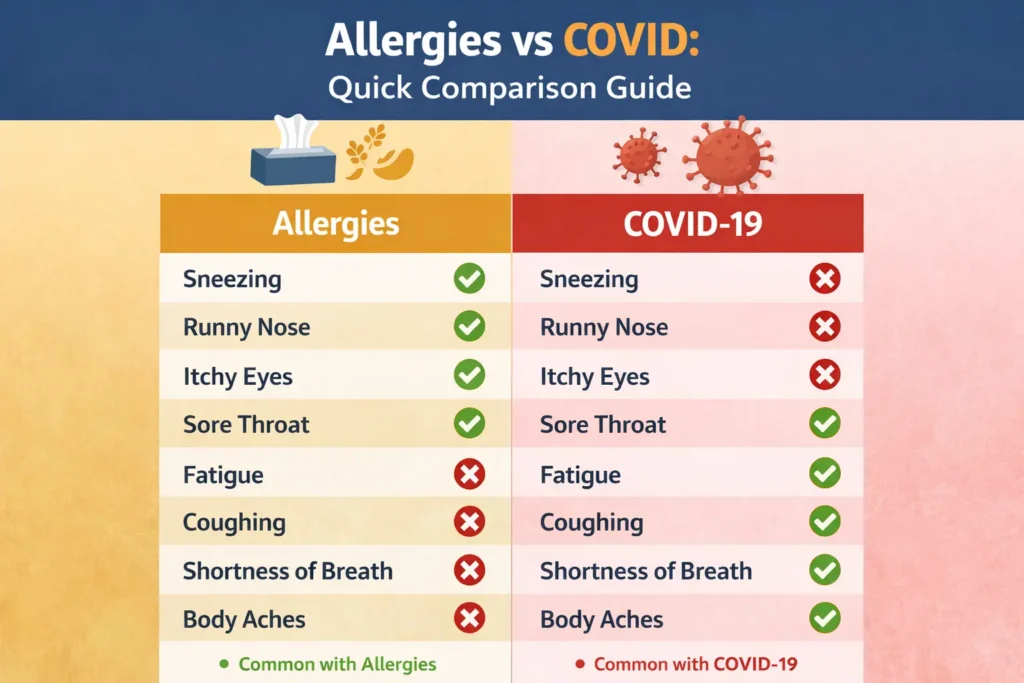
Allergies are more likely when:
- itching is prominent
- sneezing is frequent
- watery eyes are present
- symptoms follow a known trigger
- the pattern feels seasonal or familiar
- there is no fever
COVID is more likely when:
- fever or chills are present
- smell or taste changes happen suddenly
- body aches appear
- the cough is dry and persistent
- the symptoms feel more systemic
- you had a known exposure
When to seek medical care
Do not rely only on home judgment if symptoms become more serious.
Get medical help if you have:
- worsening shortness of breath
- chest pain
- confusion
- persistent high fever
- dehydration
- severe weakness
- any sign that breathing is becoming difficult
These symptoms need attention, whether the cause is COVID or something else (CDC, 2025).
Final takeaway
The best way to tell the difference between allergies and COVID is to look at the full symptom pattern, not one symptom in isolation.
Think more about allergies when the pattern is:
- itchy
- sneezy
- watery
- seasonal
- trigger-related
- without fever
Think more about COVID when the pattern is:
- febrile
- sudden
- systemic
- smell-loss related
- exposure-linked
- more intense overall
If you want the shortest version possible, it is this:
Itching points more toward allergies. Fever and sudden smell loss point more toward COVID.
That is still one of the most practical and reliable ways to tell the difference (Sarhan, R. M., et al. 2021).
Medical Disclaimer
This content is for informational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment. Always consult a qualified healthcare provider for any medical concerns or symptoms.
Frequently Asked Questions (FAQs)
1. How can I quickly tell if it’s allergies or COVID?
Look at the overall symptom pattern.
- Allergies are more likely if you have itching, sneezing, watery eyes, and symptoms that follow pollen, dust, or pet exposure.
- COVID is more likely if you have fever, body aches, sudden smell or taste loss, or feel sick overall.
2. Can allergies cause fever like COVID?
No, allergies do not usually cause fever.
If fever is present, an infection such as COVID is more likely than simple seasonal allergies.
3. Does COVID cause itchy eyes or sneezing like allergies?
COVID can sometimes cause mild nasal symptoms, but itchy eyes and repeated sneezing are much more typical of allergies.
If itching is the main symptom, allergies are usually more likely
4. Is loss of smell always COVID?
Not always.
A blocked nose from allergies can reduce smell, but a sudden and noticeable loss of smell or taste is more concerning for COVID.
5. How long do symptoms last in allergies vs COVID?
Allergies can last for days, weeks, or even months as long as the trigger remains present.
COVID usually behaves more like an acute illness and often improves over days to a couple of weeks, although some symptoms may last longer.
References
- Sarhan, R. M., El-Garhy, L. H., El-Gendy, A. O., & Ali, M. A. M. (2021). Differential clinical diagnosis and prevalence rate of allergic rhinitis and COVID-19. International Journal of Clinical Practice. https://doi.org/10.1111/ijcp.14532
- Yang, X., Zhao, J., Sima, Y., et al. (2023). Allergic rhinitis and COVID-19 association. Allergy. https://doi.org/10.1111/all.15823
- Mitchell, M. B., Workman, A. D., et al. (2023). Smell and taste loss in COVID-19. The Laryngoscope. https://doi.org/10.1002/lary.30802
- Chen, C., Song, X., et al. (2024). Allergic conditions and COVID-19 outcomes. Annals of Allergy, Asthma & Immunology. https://doi.org/10.1016/j.anai.2024.01.011
- Centers for Disease Control and Prevention. (2025). COVID-19 symptoms. https://www.cdc.gov/covid/signs-symptoms/index.html

