Post-Nasal Drip: Is It Allergies or an Infection?
Written by: Dr.Muhammad Ihsan Ullah, PhD
Medically reviewed by: Dr Ali Raza Dogar ,MBBS,ENT
Last updated on March 28,2026
That constant need to clear your throat.
The feeling of mucus sliding down the back of your nose.
The cough that seems worse at night.
The irritation in your throat that just will not go away.
If this sounds familiar, you are not alone.
Post-nasal drip is one of the most common upper airway complaints. It can happen when extra mucus collects in the nose or sinuses and drains down the back of the throat. On its own, post-nasal drip is not a diagnosis. It is a symptom. The real question is what is causing it: allergies, a viral illness, sinus inflammation, or a bacterial infection. Recent reviews emphasize that post-nasal drip is commonly linked with allergic rhinitis, nonallergic rhinitis, acute rhinosinusitis, chronic rhinosinusitis, and sometimes reflux-related conditions as well (Smallwood et al., 2024).
This is why so many people ask:
Is my post-nasal drip from allergies, or is it an infection?
That is exactly the question this article answers.
You will learn how to tell whether post-nasal drip is allergies or an infection, what symptoms matter most, what mucus can and cannot tell you, how long symptoms usually last, when allergies can increase the risk of sinus infection, and when it is time to see a doctor.
How to Tell If Post-Nasal Drip Is Allergies or an Infection
The fastest way to tell the difference is to look at the whole symptom pattern, not just the drip itself.
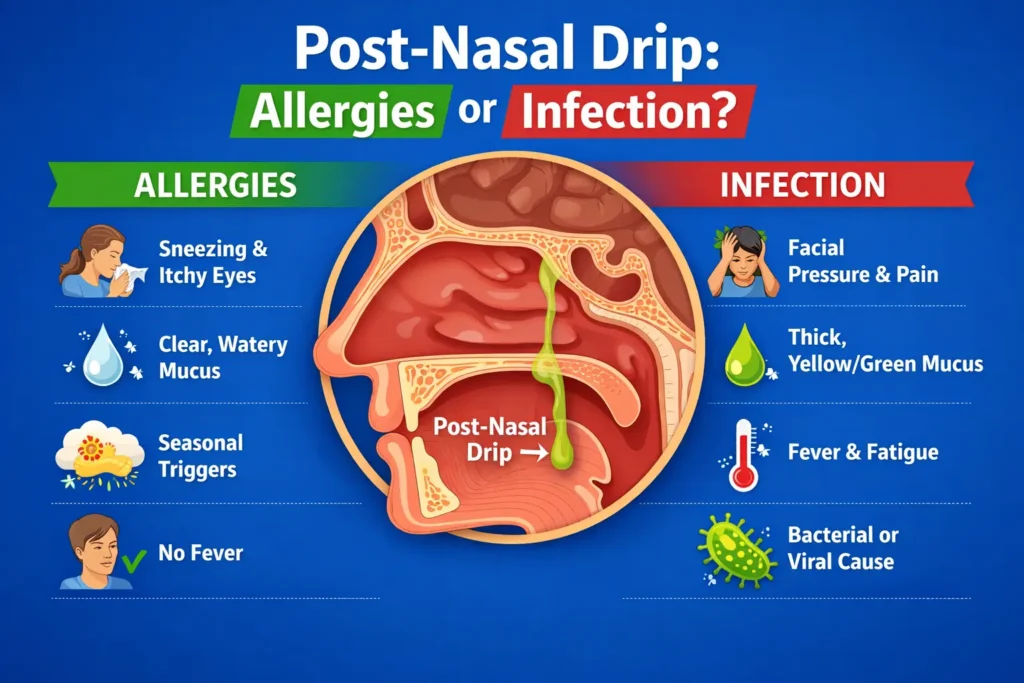
Post-nasal drip is more likely related to allergies when it comes with:
- sneezing
- itchy nose
- itchy throat
- itchy or watery eyes
- clear, watery drainage
- symptoms triggered by pollen, dust, mold, or pets
- repeated or seasonal flare-ups
- no fever
Post-nasal drip is more likely related to infection when it comes with:
- facial pain or pressure
- worsening congestion
- thick mucus
- reduced sense of smell
- headache
- upper tooth discomfort
- fever
- feeling unwell
- symptoms that started after a cold
- symptoms that last too long or get worse after seeming to improve
Recent reviews of allergic rhinitis note that classic allergy symptoms include nasal congestion, rhinorrhea, postnasal drainage, sneezing, and itching of the eyes, nose, and throat, while sinus infection guidance emphasizes persistent symptoms, facial pain or pressure, nasal obstruction, and worsening illness patterns as more concerning for rhinosinusitis rather than simple allergy alone (Bernstein et al., 2024; Payne et al., 2025).
So in simple terms:
Itching and sneezing point more toward allergies.
Pain, pressure, fever, and worsening illness point more toward infection.
Allergy vs Infection: The Fastest Clues
1.Clear drainage vs thick mucus
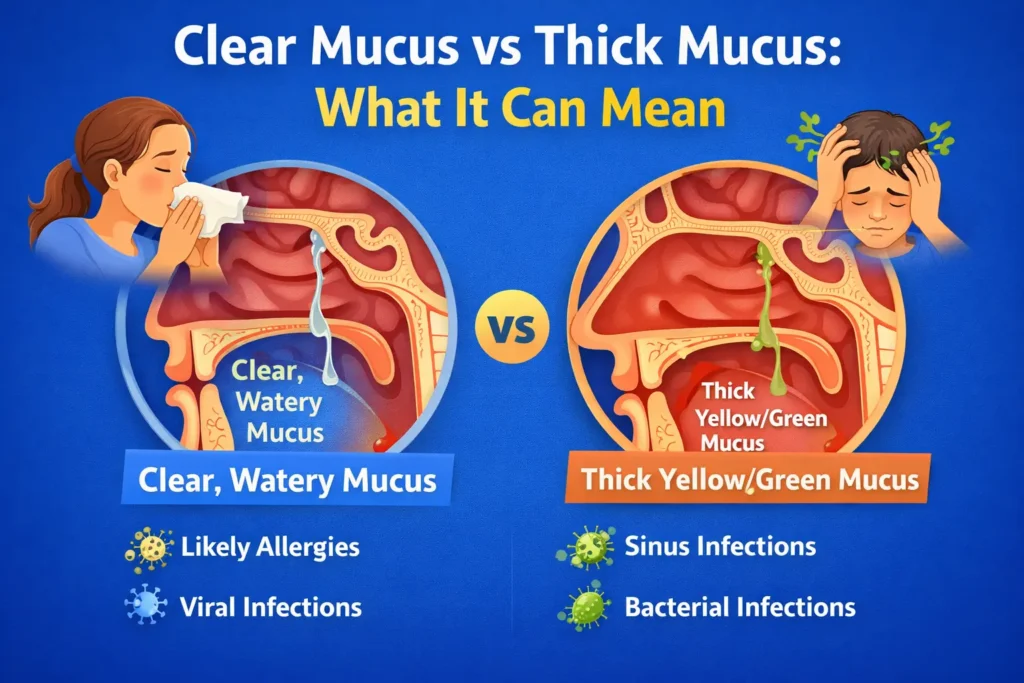
People often focus first on the mucus.
That makes sense.
But mucus should be interpreted carefully.
Allergy-related post-nasal drip often causes:
- clear drainage
- thin mucus
- watery secretions
Infection-related post-nasal drip may cause:
- thicker mucus
- cloudy mucus
- more intense congestion
- a heavier feeling in the nose and sinuses
Still, there is one very important medical point:
Mucus color alone does not prove a bacterial infection.
A person can have thick or discolored mucus during a viral illness too. That means yellow or green mucus may raise suspicion, but it should never be used alone to decide that someone definitely has a bacterial sinus infection. Modern rhinosinusitis guidance stresses that diagnosis depends on the overall pattern, severity, and duration of symptoms, not on mucus color by itself (Payne et al., 2025).
So if you are wondering about clear drainage vs thick mucus, think of it like this:
- clear and watery leans more toward allergy
- thick and heavy leans more toward infection or significant inflammation
color alone is not enough to diagnose a bacterial infection
2.Itching strongly favors allergies
This is one of the most useful clues.
If your post-nasal drip comes with:
- itchy nose
- itchy throat
- itchy eyes
- sneezing fits
- watery eyes
then allergies move much higher on the list.
That pattern fits histamine-driven allergic inflammation, which is very typical of allergic rhinitis. In contrast, infections are more likely to cause congestion, facial discomfort, pressure, and a more generally sick feeling rather than prominent itching (Bernstein et al., 2024).
So if someone asks:
Is post-nasal drip a sign of allergies?
The answer is:
It can be — especially when it comes with itching, sneezing, and watery eyes.
3.Facial pressure or pain suggests sinus involvement
If post-nasal drip comes with:
- pressure in the cheeks
- pain in the forehead
- upper tooth pain
- sinus fullness
- headache that worsens when bending forward
- reduced smell
then a sinus process becomes more likely.
This does not automatically mean a bacterial infection, because viral sinus inflammation can also cause these symptoms. But it does make infection-related sinus inflammation more likely than simple allergy alone, especially if the symptoms are persistent or worsening (Payne et al., 2025).
4.Fever is unusual with uncomplicated allergies
Allergies can absolutely make you miserable.
They can disrupt sleep.
They can leave you congested, mouth-breathing, and constantly clearing your throat.
But allergies do not usually cause fever.
If post-nasal drip comes with fever, body aches, worsening malaise, or a stronger sense of being ill, infection becomes more likely. That does not always mean bacterial infection, because many viral illnesses can do this too, but it makes pure allergy less likely (Payne et al., 2025)
What Allergy-Related Post-Nasal Drip Usually Feels Like

When post-nasal drip is driven by allergies, the story often sounds familiar.
It may start when pollen counts rise.
It may flare after cleaning a dusty room.
It may worsen around pets, mold, or smoke.
It often comes with:
- repeated sneezing
- clear or watery nasal drainage
- itchy nose or throat
- itchy, red, or watery eyes
- throat clearing
- mild cough caused by drainage
- symptoms that recur in a pattern
Allergic rhinitis remains one of the most common causes of recurrent postnasal drainage, and modern reviews continue to describe postnasal drainage, rhinorrhea, itching, and sneezing as core symptoms of the condition (Bernstein et al., 2024).
Common triggers include:
- pollen
- dust mites
- mold
- pet dander
- smoke
- perfumes or irritants
- seasonal changes
A major clue is that the symptoms often repeat under similar exposures.
That repeating pattern is very different from the usual course of an infection.
What Infection-Related Post-Nasal Drip Usually Feels Like
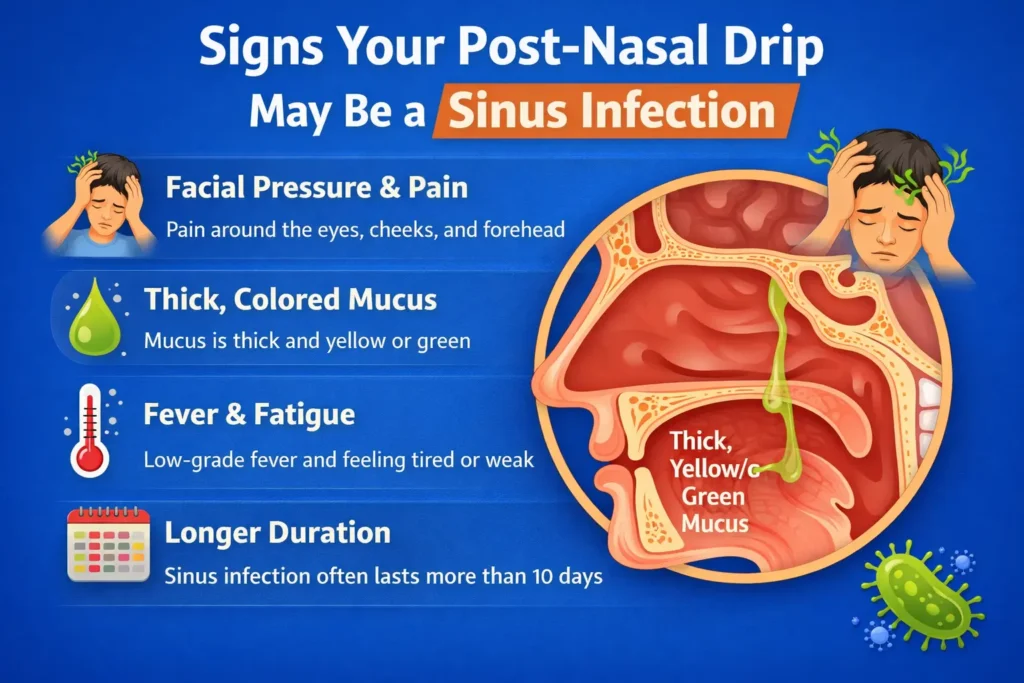
When post-nasal drip is related to infection, the pattern is often different.
Many people describe it like this:
“It started like a cold.”
“Then my nose became more blocked.”
“The mucus got thicker.”
“Now there is pressure in my face.”
“I thought I was improving, then I got worse again.”
That sequence matters.
Common features of infection-related post-nasal drip include:
- symptoms beginning after a cold
- thick nasal drainage
- marked congestion
- facial pain or pressure
- headache
- reduced sense of smell
- cough from drainage
- fever in some cases
- fatigue or feeling run down
- worsening symptoms rather than gradual recovery
Recent sinusitis guidance continues to support a practical clinical rule:
A bacterial sinus infection becomes more likely when:
- symptoms last 10 days or more without improvement, or
- symptoms get worse after initially improving, or
- symptoms are unusually severe from the start (Romano et al., 2025).
That second pattern is especially important.
It is often called double worsening.
The “Double Worsening” Pattern
This pattern is one of the most helpful clues when deciding whether post-nasal drip is related to a sinus infection.
It usually looks like this:
- You catch a cold.
- You start to improve.
- Then suddenly:
- congestion gets heavier
- facial pressure gets worse
- drainage becomes thicker
- you feel sicker again
That pattern raises concern for acute bacterial rhinosinusitis more than a steadily improving viral illness does. Current adult sinusitis guidance specifically highlights worsening after initial improvement as one of the key clinical patterns that should raise suspicion (Payne et al., 2025).
How Long Post-Nasal Drip Lasts With Allergies vs Infection
Duration matters.
Sometimes it matters a lot.
Allergy-related post-nasal drip
Allergy-related drainage may continue:
- for weeks
- through an entire allergy season
- whenever exposure continues
- off and on in a repeating pattern
It may be persistent, but it usually behaves in a way that matches environmental triggers.
Viral infection-related post-nasal drip
A viral upper respiratory illness often improves gradually over 7 to 10 days, even though cough or mild drainage can sometimes linger a bit longer while recovery continues (Romano et al., 2025).
Bacterial infection-related post-nasal drip
A bacterial sinus infection becomes more likely when symptoms:
- last more than 10 days without improvement
- become worse after improving
- are severe or progressive rather than slowly resolving (Payne et al., 2025).
So if you are asking whether post-nasal drip lasting more than 10 days could mean a sinus infection, the answer is:
Yes, especially if it is not improving or if it worsens after an initial recovery.
Can Allergies Lead to a Sinus Infection?
Yes, they can increase the risk.
Not because allergies magically transform into bacteria.
But because allergies can create the kind of inflammation that makes sinus drainage harder.
When allergies inflame the inside of the nose, they can cause:
- swelling of the nasal lining
- narrowed drainage pathways
- congestion
- mucus retention
That combination can make it easier for sinus problems to develop. Current reviews continue to recognize allergic inflammation as an important contributor to sinonasal dysfunction and symptom overlap with rhinosinusitis (Smallwood et al., 2024).
So the medically accurate answer is:
Allergies do not directly become an infection, but allergy-related swelling can make sinus blockage and secondary infection more likely.
Why Post-Nasal Drip Can Cause Throat Clearing and Cough
Many people focus only on the nose.
But post-nasal drip often bothers the throat just as much.
You may notice:
- repeated throat clearing
- a tickling sensation
- nighttime coughing
- hoarseness
- a feeling that something is stuck in the throat
This happens because the sensation of mucus drainage can irritate the upper airway and trigger coughing or repeated throat clearing. Recent reviews describe postnasal drip, also called upper airway cough syndrome in some settings, as a common contributor to chronic cough complaints (Donaldson, 2023; Smallwood et al., 2024).
That is why many people search for answers after weeks of “just clearing the throat.”
Treatment Depends on the Cause
One of the biggest mistakes in health content is treating every kind of post-nasal drip the same way.
The better approach is to match treatment to the most likely cause.
If Post-Nasal Drip Seems More Likely Due to Allergies
Helpful treatment options may include:
- intranasal corticosteroid sprays
- second-generation oral antihistamines
- intranasal antihistamines
- allergen avoidance when possible
- saline nasal irrigation
- medical evaluation if symptoms are recurrent or persistent
Recent reviews support intranasal corticosteroids as a leading treatment for persistent or more troublesome allergic rhinitis, while antihistamines can help especially with itching, sneezing, and runny nose (Bernstein et al., 2024).
More recent evidence also supports combination intranasal therapy in selected patients. A 2024 systematic review and meta-analysis found that intranasal antihistamines and corticosteroids can provide additional benefit in allergic rhinitis management, particularly when symptoms are not controlled with simpler treatment alone (Sousa-Pinto et al., 2024).
Practical points
- Antihistamines are especially useful when itching and sneezing are prominent.
- Nasal steroid sprays are especially helpful for inflammation and congestion.
- Medicines often work best when used consistently and correctly, not only on random bad days.
If Post-Nasal Drip Seems More Likely Due to Infection
Supportive care may include:
- fluids
- rest
- saline irrigation
- symptom monitoring
- medical assessment when symptoms are prolonged, severe, or worsening
For bacterial sinus infection, treatment decisions depend on severity and clinical pattern. Updated adult sinusitis guidance continues to support careful diagnosis and a selective approach to antibiotics rather than assuming every sinus complaint needs one (Payne et al., 2025; Romano et al., 2025).
That is important because most early sinus infections are viral, not bacterial.
So thick mucus alone is not a reason to rush into antibiotics.
A stronger approach is to look at:
- duration
- worsening pattern
- facial pain or pressure
- fever
- overall severity
Saline Rinses Can Help
Saline rinses can be useful for both allergy-related and infection-related post-nasal drip.
They may help:
- thin secretions
- wash out irritants
- reduce crusting
- improve drainage
- ease congestion
They do not cure the underlying cause, but they can make symptoms easier to manage as part of a broader treatment plan.
When to See a Doctor
You should seek medical care if:

- symptoms last more than 10 days without improvement
- symptoms get worse after starting to improve
- you have significant facial pain or pressure
- you develop fever
- your symptoms keep coming back
- your cough or drainage lasts for weeks
- you have trouble breathing, swelling around the eyes, or severe headache
- you are not sure whether the problem is allergy, sinus infection, reflux, or something else
Persistent or repeated symptoms deserve proper evaluation because post-nasal drip can overlap with allergic rhinitis, chronic rhinosinusitis, reflux-related throat symptoms, and other upper airway conditions (Smallwood et al., 2024).
Quick Comparison: Allergies or Infection?
More likely allergies
- clear, watery drainage
- sneezing
- itchy nose
- itchy throat
- itchy, watery eyes
- seasonal or trigger-based pattern
- no fever
- feels irritating, but not usually like a whole-body illness
More likely infection
- started after a cold
- thicker mucus
- heavy congestion
- facial pressure or pain
- headache
- reduced smell
- possible fever
- symptoms that do not improve
symptoms that worsen after initial recovery
Frequently Asked Questions (FAQs)
1. Is post-nasal drip usually caused by allergies or infection?
It can be caused by both. Allergies are more likely if you have itching, sneezing, and clear drainage, while infection is more likely if you have facial pressure, fever, thick mucus, or symptoms that worsen over time.
2. How can I tell if post-nasal drip is from allergies?
Post-nasal drip is more likely due to allergies when it comes with itchy eyes, itchy throat, sneezing, and clear watery mucus, especially after exposure to pollen, dust, mold, or pets.
3. Does thick or colored mucus always mean a sinus infection?
No. Thick, yellow, or green mucus can also happen with a viral cold. Mucus color alone does not confirm a bacterial sinus infection.
4. Can allergies lead to a sinus infection?
Yes. Allergies can cause swelling and blockage in the nasal passages, which may increase the risk of developing a sinus infection.
5. When should I see a doctor for post-nasal drip?
You should see a doctor if symptoms last more than 10 days without improvement, get worse after getting better, or come with fever, facial pain, or repeated sinus problems.
Medical Disclaimer
This content is for educational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment. Always consult a qualified healthcare professional for symptoms, concerns, or treatment decisions.
References
- Bernstein, J. A., Davis, B. P., Picard, J. K., & Cooper, P. J. (2024). Allergic rhinitis: A review. JAMA, 331(10), 866-877. https://doi.org/10.1001/jama.2024.0530
- Payne, S. C., McKenna, M., Buckley, J., Colandrea, M., Chow, A., Detwiller, K., Donaldson, A., Dubin, M., Finestone, S., Filip, P., Khalid, A., Peters, A. T., Rosenfeld, R., Akrami, Z., & Dhepyasuwan, N. (2025). Clinical practice guideline: Adult sinusitis update. Otolaryngology–Head and Neck Surgery, 173(Suppl. 1), S1-S56. https://doi.org/10.1002/ohn.1344
- Romano, F. R., Anselmo-Lima, W. T., Valera, F. C. P., Tamashiro, E., & Borin, A. (2025). Rhinosinusitis: Evidence and experience – 2024. Brazilian Journal of Otorhinolaryngology, 91(5), 101595. https://doi.org/10.1016/j.bjorl.2025.101595
- Sousa-Pinto, B., Vieira, R. J., Brozek, J. L., Cardoso-Fernandes, A., Lourenço-Silva, N., Ferreira-da-Silva, R., Pereira, A. M., Azevedo, I., Delgado, L., Bousquet, J., Fonseca, J. A., Agache, I., & Anto, J. M. (2024). Intranasal antihistamines and corticosteroids in allergic rhinitis: A systematic review and meta-analysis. Journal of Allergy and Clinical Immunology, 154(2), 340-354. https://doi.org/10.1016/j.jaci.2024.04.016
- Smallwood, D., Ledford, D., Kennedy, D., & Lockey, R. (2024). Postnasal drip. The Journal of Allergy and Clinical Immunology: In Practice, 12(10), 2538-2545. https://doi.org/10.1016/j.jaip.2024.04.030
- Donaldson, A. M. (2023). Upper airway cough syndrome. Otolaryngologic Clinics of North America, 56(1), 147-155. https://doi.org/10.1016/j.otc.2022.09.011

